Enhancements Coming to the TRICARE Formulary Search Tool
The TRICARE Formulary Search Tool (FST) helps you easily find information about your prescription medications. You can search for a medication to see if it is covered, what rules apply, and what your copayments will be at military pharmacies, through TRICARE Pharmacy Home Delivery, or at TRICARE retail network pharmacies[1].
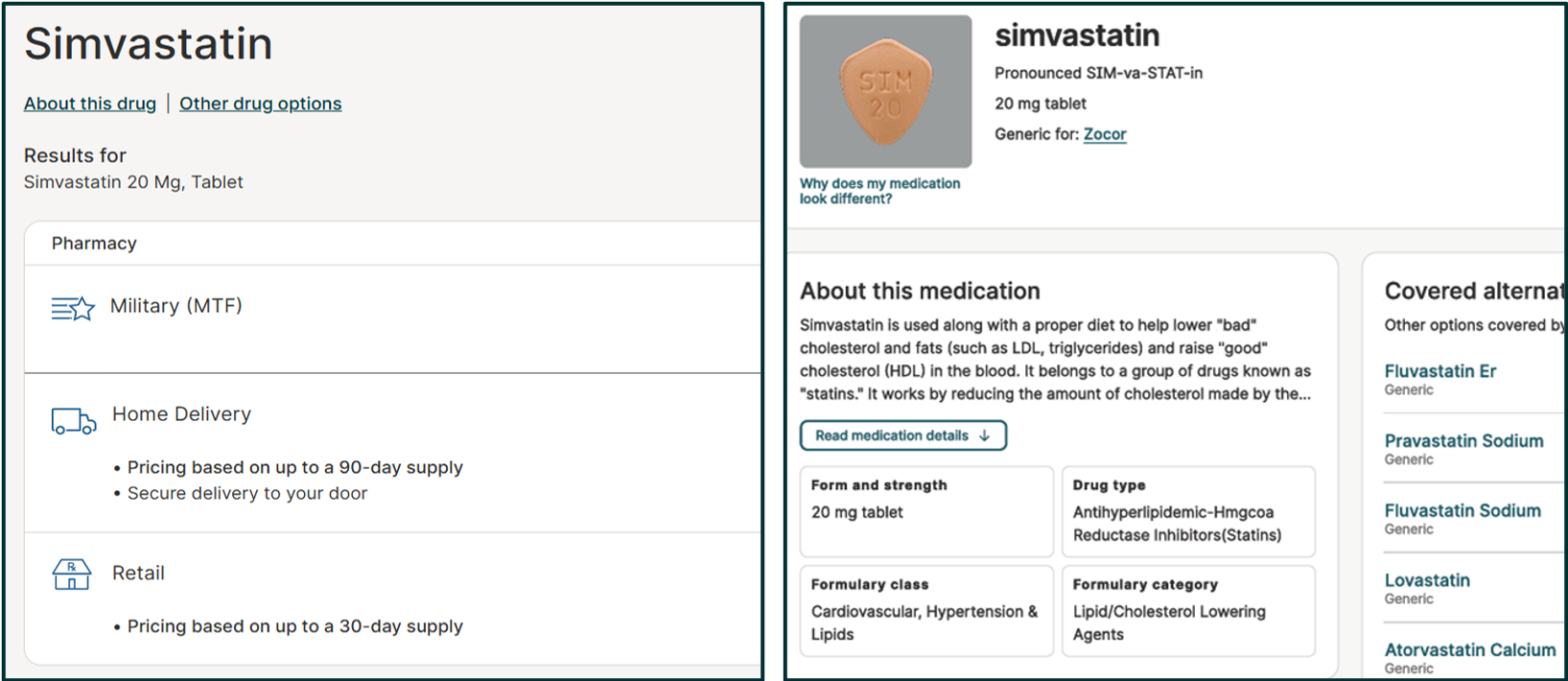
The FST is being updated to help you find information more easily. Here’s what you can expect from the improved tool:
Medication details and covered alternatives all in one place. Access essential information about your medication and covered alternatives in one convenient location. 'About this drug' and 'Other drug options' will be replaced with 'Medication details and covered alternatives.'
Quick view of coverage alerts. Select the information icon “i” to quickly see applicable coverage limitations including prior authorization, step therapy, and quantity limits.
Coverage details at your fingertips. Select “View military pharmacy/home delivery/retail coverage” hyperlink, to see coverage details and download prior authorization and medical necessity forms.
Check back soon for updates to the TRICARE Formulary Search Tool. These enhancements will help you decide where to fill your prescriptions. If you have questions about your prescription drug coverage, call us at 1-877-363-1303.
[1] At non-network retail pharmacies, beneficiaries will pay full price for their prescriptions. Beneficiaries can file a claim for reimbursement. Reimbursements are subject to deductible or out-of-network cost-shares, and copayments. All deductibles must be met before TRICARE can reimburse.
Published 4/3/2026.