Prior Authorization and Medical Necessity Basics: What You Should Know
TRICARE may require prior authorization (PA) or medical necessity (MN) to cover certain medications, including brand-name, non-formulary, or medication with coverage limitations. This process ensures the medication is effective for your condition, safe, medically necessary, and cost‑effective.
How do PA and MN work?
If PA or MN is required for your medication, your pharmacy will receive an alert. This means additional information is needed from your provider to determine if TRICARE covers the medication. Your provider will submit the required clinical information to Express Scripts for review to ensure it meets DoD Pharmacy & Therapeutics Committee established clinical criteria.
You can ask your provider to send an electronic prior authorization (ePA). An ePA is a secure, digital way for your provider to submit a prior authorization to Express Scripts. Asking your provider to fill out an ePA can help speed up the process, so you can get your medication sooner.
To learn more about medications that require a prior authorization or medical necessity, visit the TRICARE Formulary Search Tool (FST). The FST also has information about:
- Quantity and day supply limits
- Coverage and requirements
- Prior authorization and medical necessity forms
- Options for filling prescriptions and applicable copayments
- Common drug interactions and alternatives
Where can you check the status of your PA and MN?
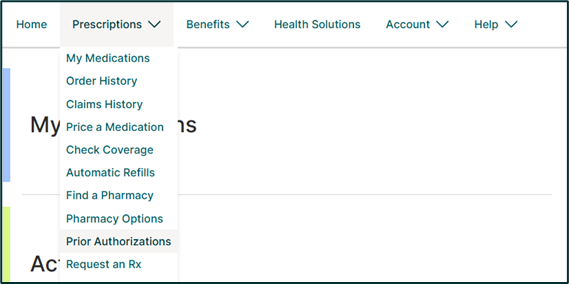
Log in to your Express Scripts online account. Under Prescriptions, select Prior Authorizations.
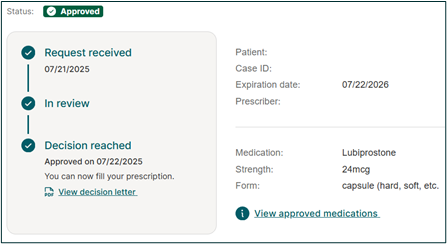
All PAs from the past 18 months will be displayed, along with the status of each request. Statuses may include Request Received, In Review, Approved, Denied, Appealed, Expiring Soon, or Expired.
You can track the status of your PA or MN from the date the request was received until a decision is made. Once a decision is reached, the approval date and expiration date will be shown, along with a copy of the decision letter. PAs and MNs can have different coverage lengths. Your decision letter will tell you exactly how long your coverage is valid.
If the PA or MN is approved and your medication is covered, your prescription will be filled.
If a PA or MN is denied, you have the option to pay out of pocket for the medication, discuss other treatment options with your provider, or file an appeal. If an appeal is submitted, you can track the status of your appeal as well as review any decision letters provided.
You can also view the prior authorizations you have on file in the Express Scripts® Pharmacy Mobile App. Select More, then Prior Authorizations.
To learn more about Prior Authorization and Medical Necessity, visit militaryrx.express-scripts.com.
Published 5/13/2026.